On this page: Zoonoses | Physical Injuries & Chemical Hazards - Precautions, Reporting & Disposal | Occupational Health Program (OHP) for Animal Related Activities | Personal Hygiene and Protection | Allergies
Working safely with experimental animals encompasses not only the people and the animals, but also the facilities, equipment, and the procedures we use. It also encompasses the community in which we each live. We must each practice safe working habits to ensure that any health risks in our working environments never "leak" into the community because of faulty procedures or carelessness. The principal investigator must assume responsibility for ensuring that personnel working on the project are aware of any risks to health and safety.
Policies and programs required under provincial Occupational Health and Safety laws and regulations are implemented by each institution. Such institutional programs must support a safe working environment in animal facilities as well.
Biological Hazards
Zoonoses
Definition: The CCAC Guide to the Care and Use of Experimental Animals defines zoonosis as a disease of animals that may under natural conditions be transmitted to humans. What this really means is a disease that it is communicable between animals and humans.
The list of potential zoonoses related to working with animals in research, teaching or testing is quite long, and numerous books have been written on the subject. (See the CCAC Guide to the Care and Use of Experimental Animals, Volume 1, 2nd Ed.. Appendix VII Zoonoses). However, in reality the risks are very low when dealing with the common small laboratory animal species in the laboratory. There are several reasons for this low risk. Firstly, commercial suppliers of laboratory animals have done an excellent job of producing disease-free animals. As well, institutions generally have developed good occupational health and safety programs that include active veterinary monitoring and care programs.
The risk of working with highly infectious agents is significantly reduced when using a bio-safety cabinet, proper personnel protective equipment (PPE) and biohazard training.
The use of proper PPE not only protects the user, but the animals as well.
The risk of exposure to zoonotic diseases is greater for those who work with experimental animals from random sources (including cats, dogs and most livestock), and for field researchers studying wild animals in their habitat. Working with non-human primates in the laboratory is a special case because of the many zoonotic concerns.
A few of the most common zoonoses in each of these areas of animal research will be presented as examples. For more information on zoonoses, and for more information about specific disease organisms, the Material Safety Data Sheets (MSDS) for individual organisms published by Health Canada Office of Laboratory Security can be consulted.
Routes of Exposure
Common routes of exposure to infectious organisms are:
- aerosol (inhaling the organisms)
- ingestion (swallowing the organisms)
- absorption through the skin, through mucus membranes or skin wounds
- injection (accidental, in research)
The use of appropriate equipment, including personal protective equipment appropriate to the route of exposure for a particular infectious organism, and appropriate practices, will minimize the risk of exposure.
Zoonoses Associated with Commercially Produced Laboratory Animal Species
As noted above, the risk of exposure to a zoonosis while working with common small laboratory animals that are commercially reared is very small. One example is presented here: Rat bite fever.
Rat Bite Fever
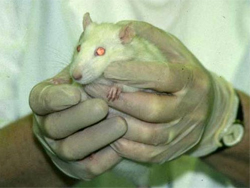
- Organism name, and synonyms: Streptobacillus moniliformis, a Gram-negative bacteria. Synonyms: Rat-bite fever, Haverhill fever.
- Reservoir: Rats. Commensal in the mouth and pharynx.
- Mode of Transmission: Animal bite, direct contact with secretions of the mouth, nose, eye of an infected animal.
- Incubation Period: 3-10 days.
- Clinical Disease: Initial bite wound usually heals. Sudden onset of fever, chills, vomiting, headache and joint pains, rash.
- Epidemiology: Uncommon in North America.
- Communicability: Not directly transmitted from person to person.
Zoonoses Associated with Random Source Laboratory Animal Species
Ringworm

Ringworm is a fungal infection of the skin that can occur in a wide range of animals including humans.
- Organism names, and synonym: Microsporum spp., Trichophyton spp., fungal organisms. Synonyms: Ringworm, dermatomycosis, tinea.
- Reservoir: Most domestic and wild animals, and humans. May be latent in hair of some species.
- Mode of Transmission: Direct or indirect contact with skin lesions or infected hair, or fomites (brushes, clippers, etc.).
- Incubation Period: 4-10 days.
- Clinical Disease: The fungi infect keratinized areas of the body - hair, skin and nails. Signs include round lesion of scaling skin, hair loss or breakage, sometimes reddened and crusting of infected skin.
- Communicability: Communicable from person to person when infective lesions are present.
- Diagnosis and Prevention: Monitoring for typical signs, confirmed by skin scrapings and culture. Many treatments are available.
Rabies

Rabies can infect any mammal, including humans. Purpose-bred laboratory animals are not a likely source of rabies. However wild animals, animals obtained from random sources, or livestock, may carry rabies. Many institutions have rabies vaccination policies for at-risk personnel.
- Organism name, and synonym: Rabies - a rhabdovirus, Rabies, Hydrophobia.
- Reservoir: Wild and domestic animals (e.g., dogs, cats, foxes, coyotes, skunks, racoons) and bats.
- Livestock and rodents may be secondary hosts if infected by a biting animal.
- Mode of Transmission: Most commonly by a bite which introduces the virus from the saliva of a rabid animal. May be airborne in caves inhabited by infected bats.
- Incubation Period: Usually a few weeks, but may be up to a year or longer. The virus propagates in nerves. Thus the site of the wound (distance from the brain), presence of nerves at the wound, etc., influence the incubation period.
- Clinical Disease: Once clinical signs appear, the clinical course is short - usually less than 10 days with death due to respiratory paralysis. Signs include apprehension, behavioural changes, spasms of swallowing muscles, delirium, weakness progressing to paralysis.
- Epidemiology: Worldwide distribution with some rabies free areas. All mammals susceptible.
- Communicability: Infected animals shed virus for a few days before clinical signs appear. From then until the death of the animal, it is infectious.
- Diagnosis and Prevention: Pre-exposure immunization of all individuals at high risk (those who will handle animals, including laboratory workers, veterinarians and other animal handlers) should be used. The human diploid cell vaccine (HDCV) is currently used. Post-exposure treatment includes immediate first aid by generously flushing the wound and washing with soap and/or antiseptics, and providing post-exposure treatments as directed by the physician (e.g. rabies immune globulin, and vaccination).
Zoonoses Associated with Farm Animal Species
Q Fever

Q Fever may be contracted from working with sheep or goats, particularly ewes during lambing. The placenta and fetal fluids contain high levels of the organism in infected ewes.
- Organism name, and synonyms: Coxiella burnetii, an intracellular bacteria. Synonyms: Q Fever, Query fever, Rickettsia.
- Reservoir: Most common in sheep, cattle, goats. Infected domestic animals usually asymptomatic but shed massive numbers of organisms at parturition, in the placenta and placental fluids.
- Mode of Transmission: Direct contact with infected animals and their birth fluids; inhalation of organisms in dust from contaminated premises; wool from sheep.
- Incubation Period: Usually 2-3 weeks.
- Clinical Disease: Sudden onset fever, chills, headache, weakness, malaise, severe sweats; pneumonia, usually self-limiting. Chronic infection mainly involves endocarditis. Up to half of infections are asymptomatic.
- Epidemiology: Worldwide distribution. Occurs in laboratories using sheep for research; cases in research staff, exposed hospital patients.
- Communicability: Direct transmission from person to person very rare.
- Prevention: Use of appropriate protective clothing including masks. Serologic monitoring of ewes of limited value. Appropriate sanitation procedures. Vaccination available.
Zoonoses Associated with the Nonhuman Primates
As noted earlier, nonhuman primates are a potential source of many zoonotic diseases, and special facilities, equipment and procedures are required to work with them safely. The zoonosis discussed here - Herpes B infection - is the one that most people will have heard about.
Herpes B virus Infection
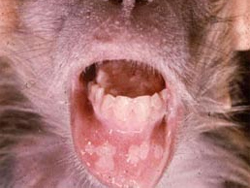
Herpesvirus simiae (B virus) causes a fatal ascending encephalitis in humans infected from old world nonhuman primates. The disease in the host nonhuman primates is usually mild or asymptomatic.
- Organism name and Synonym: Herpesvirus simiae, a DNA herpesvirus. Synonyms: B virus, Monkey B virus, Simian B disease.
- Reservoir: Common in old world monkey of the macaque group (most common in rhesus and cynomolgus macaques), both wild and captive colonies.
- Mode of Transmission: Latent infection in macaques with periodic episodes of oral lesions and shedding of virus in saliva. Transmission after a bite or direct or indirect contact with infected saliva or tissues. Laboratory infections from infected tissues can occur. Aerosol exposure minimal.
- Incubation Period: 3 days to a month.
- Clinical Disease: Acute, usually fatal, ascending encephalomyelitis; fever with headache, lesions at site of exposure. Death in 1 day - 3 weeks after onset of symptoms in over 70% of cases.
- Epidemiology: Occurs in veterinarians, laboratory workers and others handling old world monkeys or tissue cultures derived from these species.
- Communicability: Transmission from person to person rare.
- Prevention: Appropriate use of protective laboratory clothing (long sleeved lab coats, face shields or surgical masks and goggles or glasses), proper methods of restraint.
The zoonotic diseases associated with reptile and amphibian contact are primarily bacterial infections. These include Salmonella, Mycobacterium, Campylobacter, Aeromonas, Escherichia coli, Klebsiella, Serratia and Flavobacterium meningosepticum.
Zoonoses Associated with Wild Animals and Field Studies
Hantavirus Infection

- Organism name, and synonym: Hantavirus, an RNA virus in the Bunyavirus family. Synonyms: hantavirus, hantavirus pulmonary syndrome (HPS), Sin Nombre Virus (SNV) in North America.
- Reservoir: Wild rodents such as Peromyscus (deer mouse) and Microtus species in the Americas.
- Mode of Transmission: Inhalation of the virus in the dust from areas where infected rodent excreta (urine and feces) are present is the most common route. Rodent bites may transmit the disease.
- Incubation Period: Average two to four weeks but may be shorter or longer.
- Clinical Disease: Hantavirus Pulmonary Syndrome (HPS) is characterized by a sudden onset fever, pain, vomiting, and onset of respiratory distress and prostration. Mortality rates are high despite symptomatic treatment.
- Epidemiology: Occurs throughout much of North America including the western provinces.
- Communicability: Not thought to be communicable between persons.
- Diagnosis and Prevention: Use of personal protective equipment to avoid inhaling the dust particles with virus, and other direct contact in high risk areas should be used. Field biologists and persons working in previously "contaminated" buildings are at risk. Guidelines for protection against infection and for decontaminating facilities are available at the CDC (Centers for Disease Control and Prevention) web site.
Physical Injuries & Chemical Hazards - Precautions, Reporting & Disposal
Physical injuries related to the handling of animals may be kept to a minimum by ensuring that:
- everyone is trained and experienced in handling the species with which he works, and that he knows the particular hazards associated with each species;
- everyone is familiar with the hazards of the experiment, and is provided with (and use) a proper working area, protective clothing and equipment;
- a mechanism is in place in every unit to deal with animal-inflicted injury, and for referral for any further medical treatment if this is required.
Many tasks in animal facilities require moderate to heavy physical labour, and performing these tasks may expose personnel to risks from moving heavy equipment (strains), slippery floors, electrical hazards when washing, noise, etc. Each person must exercise due caution when performing such tasks.
Although the importance of understanding basic animal behaviour in the human/experimental animal interaction to avoid injuries can be emphasized here, it cannot replace the skills that are learned by working directly with the animals. Skilled animal care technical staff will already have the right attitudes and approaches towards animal handling and manipulations. They will also have the practical skills to do so safely and humanely. For others, some of the material presented here can serve as a useful introduction to handling animals safely in an experimental animal facility.
To work safely with an experimental animal a person should:
- understand basic animal behaviour in relation to their interactions with people during handling
- appreciate the "flight zones" typical of a species
- understand how to communicate with the animal
- use appropriate restraint techniques
- use restraint equipment properly
- identify any animals that may be unpredictable
- wear appropriate protective clothing and equipment
- maintain appropriate vaccination status
The ultimate way for a positive impact on both animal users and the research animals are institutional sentinel, monitoring and quarantine programs.
Occupational Health Program (OHP) for Animal Related Activities
Activities involving the care and use of animals in research and teaching pose particular health risks not normally encountered in other activities. The magnitude of risk is dependent on:
- the nature of contact (direct or indirect) with animals, their tissues, excreta, body fluids, hair, animal cages, dander and
- the species involved.
In recognition of its responsibility to provide a safe working environment, McGill University has adopted this policy for protection of faculty, staff, and students from health risks which may result from working with animals or working in animal care activities. Please see the Occupational Health Program website.
Objectives
- Protection of individuals from hazards associated with animal care and use.
- Ensuring that individuals are thoroughly informed of the risks associated with their work.
- Provision of preventative medical services and delivery of prompt and adequate medical care and advice.
- Rehabilitation of employees whose health has been compromised due to occupational exposures.
- Ensuring that individuals are physically able to perform their assigned tasks without undue risk to themselves or fellow workers.
- Protection of animals from diseases they may contract from humans.
General Statement of Policy
- education and training,
- isolation and containment of high risk activities,
- evaluation of health status prior to exposure,
- periodic health assessment,
- provision of emergency health care,
- administration of immunization or other prophylaxis for protection from specific risks,
- exclusion of unauthorized persons from animal facilities,
- exclusion of persons with active infectious diseases that are hazardous to fellow workers or to animals,
- use of appropriate apparel, equipment, and facilities,
- veterinary management of animal health, and
- maintenance of records of illnesses, occupational diseases and injuries.
This policy requires confidentiality in the handling of medical information. Individuals required to undergo any medical examinations, treatment, or monitoring must be fully informed of the associated benefits and risks.
The services are to be provided at no cost to the individual. All activities related to this program are to be available during normal working hours.
Education and Training
Persons working with animals or in animal facilities should be fully informed as to the nature of possible risks associated with proposed duties. It is the responsibility of each laboratory director to inform research personnel of the specific risks involved and the applicable procedures.
Training in the principles of radiation and chemical safety is the responsibility of the local Environmental Safety Office. In Canada, the use of radioisotopes is controlled by the Canadian Nuclear Safety Commission.
Medical Care Elements of Program
This section is applicable to routine health surveillance activities involving animal care and use. Animal bites or other accidents involving animals are not covered in this section and should be considered for emergency treatment.
Registration
IF YOU ARE WORKING IN A HOSPITAL OR HOSPITAL RESEARCH INSTITUTE, please contact your local Health Office.
McGILL UNIVERSITY NON-HOSPITAL-RESEARCH-INSTITUTE members may apply to the Occupational Health Program for Animal Related Activities by going to the Environmental Health and Safety website.
Personal Hygiene and Protection
Protective clothing suitable for the handling to be done should be worn at all times; laboratory coats, coveralls, gloves, masks, boots (e.g., steel-toed for working with cattle), etc. As noted above, the handling of non-human primates is a special situation that requires special protective clothing.
Allergies
Laboratory animal allergy (LAA) may be the most prevalent occupational hazard facing people working in experimental animal facilities. Surveys have revealed that up to 44% of people working with laboratory animals develop allergies to one or more species, and they usually become allergic within 3 years of first exposure (range; 1 month to 9 years).
Allergic reactions can be classified according to the site of the reaction: upper respiratory; lower respiratory; skin; generalized, anaphylactic.
In any individual, several symptoms may occur. The upper respiratory symptoms are the most common - up to 80% of affected people experience symptoms such as itchy, runny nose and eyes, and sneezing. About 20-30% of affected people experience lower respiratory symptoms, some progressing to occupational asthma. There is shortness of breath due to bronchoconstriction and airway mucus production. Asthma may become life-threatening if not treated. About 40% of laboratory animal allergic people experience skin reactions upon contact with the animal or the allergens. Much more rare, fortunately, is the acute generalized reaction (anaphylaxis) requiring emergency treatment. There are only a few documented cases of anaphylactic reactions to laboratory animal bites (e.g., rat bites).
Almost all species of common laboratory animals can trigger an allergic reaction. Allergies to the rat, rabbit, mouse, guinea pig, cat and dog are the most common.
The animal allergens are mostly small molecular weight proteins such as albumen. These proteins occur in the serum and tissues, but also in the saliva, urine and skin dander. When animals groom themselves, the salivary proteins also end up on the skin, and on the dander particles that flake off and become aerosolised.
Risk Factors for Becoming Allergic to Laboratory Animals
The risk factors for becoming allergic to laboratory animal allergens include atopy, smoking, gender and intensity of exposure.
There is a correlation between atopy (an inherited, familial tendency to develop some form of allergy such as hay fever, asthma, eczema) and the potential for developing LAA, and a stronger positive correlation between atopy and development of lower respiratory symptoms (asthma). Pre-employment health screening may be useful to identify atopic individuals.
Smoking reportedly does not increase the risk of developing LAA, but if a smoker does develop LAA, they are 1.5-3 times as likely to get the lower respiratory symptoms (asthma).
Males are more likely to be atopic than females (47% vs 37%) and so more likely to develop LAA.
There is a strong correlation between the intensity of exposure to the allergen, and the severity of symptoms. However, any allergen exposure, even very low levels, will trigger symptoms in allergic individuals.
Factors Affecting Animal Allergen Levels in Laboratory Animal Rooms
Ventilation and Relative Humidity
Directional room ventilation, negative flow laminar ventilated cage racks, or ventilated racks assist in reducing particles in room air. Low relative humidity results in higher dust and allergen levels. A relative humidity of 50-65% significantly reduces the quantity of allergen being aerosolized. Do the same air quality standards apply to rooms where animals are housed in ventilated racks? Yes, the air quality standards for the room are the same, regardless of the equipment in the room. Although individually ventilated cages have a much higher air change rate (i.e. 30-70 air changes per hour) than the room, the air supply for ventilated cages is often drawn from the room. In these cases, the animals are susceptible to the air quality conditions of the room. Even if the air entering the cages is high efficiency particulate air (HEPA) filtered, there is no protection for the animals against the organic and inorganic gases present in the room air, or from the heat load created from equipment and people working in the room. This type of air filter can theoretically remove at least 99.97% of dust, pollen, mold, bacteria, and any airborne particles with a size of 0.3 microns (µm). (A tenth of a micron in diameter).
Type of Bedding
Studies have shown that sawdust/wood chip bedding results in higher levels of aerosolised allergen in rodent rooms than corncob bedding. Use of processed paper products and absorbent pads result in lower levels of aerosolised allergens.
Cleaning and Sanitation Practices
A high level of cleanliness results in reduced levels of allergens circulating in laboratory animal rooms.
Animal Room Tasks Associated with Exposure to Allergens
All commonly performed animal room tasks result in significant exposure to airborne allergens and dust. Cage cleaning (and waste dumping), animal care procedures (feeding, watering, etc.), animal manipulations (e.g., handling, injections), and general room cleaning all result in significant levels of airborne allergens.
Reducing Exposure to Allergens
There are several approaches to reducing exposure to laboratory animal allergens. Housing rodents in filtered cages and ventilated cage racks, use of ventilated waste dumping stations and laminar flow hoods for animal manipulations, will all help minimize exposure to laboratory animal allergens. Maintaining a high level of cleanliness, and using a bedding type that minimizes aerosol dust particles will also help minimize exposure to laboratory animal allergens.
The appropriate use of personal protective equipment such as good quality particulate masks and gloves can significantly reduce exposure to animal allergens. Such equipment should be provided for all staff required to work in high exposure areas. As well, good personal hygiene (regular hand washing, showering, etc.) should be practised.
Institutional Responsibilities
There are several institutional responsibilities to minimize the impact of laboratory animal allergies. These include education programs for staff, health monitoring of at risk persons, improved engineering standards for ventilation and relative humidity, and provision of appropriate personal protective gear.
Education programs that cover topics such as symptoms, risks, defining risk zones and tasks, proper use of personal protective equipment, and health counselling for affected and at-risk staff, are very important.
Allergies to animals are nothing to sneeze at.