How children and families can be helped when health workers ask about their underlying social challenges
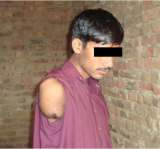
It is common practice for small family-based agricultural workers to use a fodder-chopping machine to prepare and store the feed for the animals. This electric machine found in many backyards has sharp metal blades that are very dangerous (see video clip Child labour in Pakistan below) and amputations are not infrequent. Indeed, the amputation was not Muhammed’s first work-related injury. He had previously injured his leg with a sickle while cutting grass. At that time, he went to a local village doctor who bandaged his leg and then he went back to doing the same dangerous work again. The next time he was injured, when his arm was amputated, he was bleeding profusely and went to the local hospital for treatment. He is once again, back at work on the farm, doing the same dangerous tasks, but now single-handed. Yet, the health system can do more than simply “put on band-aids.” There are many missed opportunities for prevention.
Muhammed feels that given his disability, he “should be given a government job” or some safer way to earn a livelihood. He says “I hope that I shall get an education and a good job, so that the future is good.” Muhammed further suggests that frontline health workers “should take care of the poor patients too and

This is just one example of many. Moreover, we intend to build on local knowledge and experience to develop more universal principles and guidance for assisting frontline health workers in providing direct care to vulnerable children and families and in stimulating larger social change. The first phase of our work involved conducting interviews with a wide range of child labourers ranging from agricultural workers and rag pickers to street vendors and domestic workers. These children reported numerous harms related to their work, going beyond physical injuries, to include financial exploitation, psychological trauma, discrimination and sexual abuse, not to mention having to abandon their studies and jeopardizing their chances of obtaining an education and improving their prospects for the future. Interviews with various health workers and community stakeholders revealed particular concern regarding children who get caught up in illicit activities such as working in the drug trade (particularly in Brazil) or who are sexually exploited as child prostitutes. In Niger, children are even involved in mining for gold and risk falling over 70 feet to their death in an open pit (see video clip Child Labour in Niger below). Yet, even in the face of widespread poverty, where in some countries more than 50% of children work to support their families, frontline health workers can make a difference.
The people that we interviewed had a wealth of suggestions regarding how frontline health workers can address the social causes of poor health. It is this insight that we wish to share and make more widely available. Whether they are local village doctors, midwives, dispensers or community health workers, frontline primary health care workers are in a special position to deal with sensitive issues, and they are also well placed to be able to reach out and make contact with the most marginalized and vulnerable children and families – since without contact there can be no impact. According to one frontline health worker:
“When a health worker visits homes of different people she gets to know what kinds of problems they are facing... We can go to their homes and ask them and they will tell us without any hesitation because they have faith in health workers and believe that we have come for their help. They tell us about their problems. We suggest them measures to solve their problems and if there is a need we accompany them too. This is the reason they are able to share with us everything.”
Frontline health workers are respected members of society and therefore they can share the stories of the hardships that their patients encounter and advocate for larger social change within communities and even within industry. Yet, many frontline health workers interviewed would like training and support in addressing these complex health and social issues. It needs to be an explicit part of their mandate:
“Health workers like us should be educated first. Our capacity should be increased. Then we will be able to transfer these things further. Then there will be a continuous chain system which takes us towards betterment.”
Providing this training and support to improve the health of vulnerable and marginalized children and families is the overarching goal of the CLEAR collaboration.