We have a multitude of free resources on management of the illness, aspects of care, caregiving and other related topics.


A common stomach bacteria found in two thirds of the world population may be linked to a higher risk of Alzheimer’s disease, new research suggests.

Despite extensive research and encouraging findings, Alzheimer’s disease (AD) remains difficult to diagnose based on signs and symptoms alone. But what if one day, a blood sample during an annual check-up could be used to identify the disease? A recent McGill-led study has found that a new kind of blood test is as effective at detecting AD as lumbar punctures, one of the current methods used to diagnose AD.

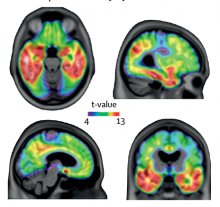
Thinning in the right temporo-parietal cortex and left prefrontal cortex were similar in both groups
A new study led by scientists at The Neuro (Montreal Neurological Institute-Hospital) of McGill University finds a correlation between neurodegeneration in obese people and Alzheimer’s disease (AD) patients.
New research at The Neuro is studying a targeted brain training program and a potential new treatment for early Alzheimer’s.
For more information on these two studies, contact the neurocognitive team at the Clinical Research Unit at The Neuro at info-cru.neuro [at] mcgill.ca or visit cru.mcgill.ca/ad_en.
What is Dementia-Friendly Canada?
The Dementia-Friendly Canada project is a partnership between the Alzheimer Societies of Canada, British Columbia, Saskatchewan, Manitoba and Ontario and is intended to foster the creation of dementia-friendly communities across the country.

This visionary support will enable the new Office of Ed-TECH to expand opportunities for online learning in dementia education and other community-based and professional training initiatives
A generous commitment of $1.5 million from the Amelia and Lino Saputo Foundation will support innovative teaching at the new Office of Ed-TECH (Education Technology and E-Learning Collaboration for Health) at the McGill Faculty of Medicine and Health Sciences (FMHS) under the umbrella of the Amelia Saputo Community Outreach for Dementia Care.

U.S. government health officials approved the first new drug for Alzheimer's disease in nearly 20 years, disregarding warnings from independent advisers that the much-debated treatment hasn't been shown to help slow the brain-destroying disease. The Food and Drug Administration (FDA) said it granted approval to the drug from Biogen based on results that seemed “reasonably likely” to benefit Alzheimer's patients. (CTV News)

Neural “signature” may reflect how we respond to feelings of social isolation
This holiday season will be a lonely one for many people as social distancing due to COVID-19 continues, and it is important to understand how isolation affects our health. A new study shows a sort of signature in the brains of lonely people that make them distinct in fundamental ways, based on variations in the volume of different brain regions as well as based on how those regions communicate with one another across brain networks.

Work will tell us how loneliness interacts with brain structure and function in normal aging and pre-symptomatic Alzheimer’s disease
Two researchers from The Neuro, with collaborators from the StoP-AD Centre at the Douglas Mental Health University Institute and the Quebec Artificial Intelligence Institute, will lead a research program centered on an emerging field of neuroscience thanks to a grant from the National Institutes of Health/National Institute of Aging (NIH/NIA) in the USA.

Findings could lead to development of pre-clinical stage therapeutics
By Jason Clement
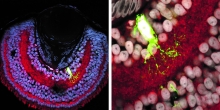
For decades researchers have known that Alzheimer’s disease (AD) causes the atrophy of a system of neurons and synapses highly involved in memory, learning and attention, which is highly dependent on a molecule known as nerve growth factor (NGF). The disease causes dysregulation of NGF’s metabolism, leading to the loss of the synapses and neurons that depend on it, akin to plants being deprived of light.
McGill-Gothenburg collaboration yields affordable test that could revolutionize the way AD is diagnosed, studied and treated
By Gillian Woodford
A simple blood test that can detect Alzheimer’s disease (AD) has been discovered and validated in a joint effort by a McGill team and researchers in Sweden. Their results are published in the May issue of The Lancet Neurology. An accompanying commentary calls the discovery “transformative.”

New technique could be used to choose best therapies for patients and measure their effectiveness
Evaluating the effectiveness of therapies for neurodegenerative diseases is often difficult because each patient’s progression is different. A new study shows artificial intelligence (AI) analysis of blood samples can predict and explain disease progression, which could one day help doctors choose more appropriate and effective treatments for patients.

McGill researchers’ findings show that may be the case

Study sheds light on longstanding debate
Researchers have known for decades that inflammation accompanies Alzheimer’s disease (AD) brain lesions. Several early studies suggested that “super-aspirins” or Nonsteroidal anti-inflammatory drugs (NSAID) could help avoid the disease. However, after clinical trials showed that NSAIDs don’t help patients who already have AD symptoms, doctors wondered whether these drugs could still be helpful to people who were at risk of developing the disease, but weren’t yet showing symptoms.
